As society becomes increasingly appearance-conscience, people are paying attention to parts of their bodies they had previously overlooked. While cosmetic surgery was most commonly used to improve and enhance the appearance of the face, the popularity of having elective cosmetic procedures has now spread throughout the body – most recently to the feet. A recent survey conducted by the American Orthopedic Foot & Ankle Society (AOFAS) among its podiatric surgeon members found that just over fifty percent of all their patients had inquired about cosmetic procedures for the feet. So why the sudden interest in cosmetic foot surgery? There are two reasons – to improve the appearance of the foot and to correct deformities of the foot.
As society becomes increasingly appearance-conscience, people are paying attention to parts of their bodies they had previously overlooked. While cosmetic surgery was most commonly used to improve and enhance the appearance of the face, the popularity of having elective cosmetic procedures has now spread throughout the body – most recently to the feet. A recent survey conducted by the American Orthopedic Foot & Ankle Society (AOFAS) among its podiatric surgeon members found that just over fifty percent of all their patients had inquired about cosmetic procedures for the feet. So why the sudden interest in cosmetic foot surgery? There are two reasons – to improve the appearance of the foot and to correct deformities of the foot.
Just like some people think their nose is too big or their breasts are too small, others find faults in their feet. Perhaps they believe their toes are too short, too long, too crooked or that their feet are just too fat. Cosmetic procedures to improve the appearance of the feet may include removing fat from toes that are too chubby, adding fat to other areas of the feet that may be too thin, surgically narrowing feet that may be too wide or microdermabrasion procedures that smooth the appearance of the feet and remove rough patches of dead or dry skin. Of course, while all of the aforementioned procedures are mere cosmetic enhancements that are purely elective, there are other cosmetic surgeries of the foot that improve that improve the appearance of the foot while correcting an underlying condition that causes the altered appearance.
Conditions like hammertoes, bunions, misaligned or broken toes and other mild deformities of the feet can not only detract from the appearance of the feet, they can also pose mobility problems in the future if left untreated. Walking may become increasingly difficult or even painful if these deformities are not addressed by surgical intervention. The cosmetic benefits of this type of foot surgery are just a perk, not the goal of the procedures.
Most cosmetic surgeries of the feet can be done on an outpatient basis where the patient goes home the same day of the procedure. Depending on what they had done, aftercare can range from hardly any limits at all imposed on activity to the need for crutches for several weeks post-op. As with any surgery, there can be some pain and discomfort after the surgery, which are both easily treated with medications.
If you have been considering cosmetic foot surgery to correct a deformity of the foot or just for cosmetic enhancement only, we invite you to schedule a consultation with our Beverly Hills podiatrist, Dr. Jamshidinia. He can create a plan of treatment, based on your wishes and the findings of the consultation, that will help you put your best foot forward in all that you do.
Email La Peer Health Systems at [email protected] today to get more information about cosmetic foot surgery procedures.
To learn about other cosmetic foot procedures offered at La Peer, please visit BunionDr.com, our site dedicated to bunion treatment and cosmetic foot procedures.
By: Kamram Jamshidinia
Next, read about Bunion Surgery.
 Going to the doctor can often times be daunting. Not only are you nervous about finding out whether or not you are healthy, but you also can be afraid that the doctor will judge you on your health, or more likely unhealthy, habits. However, you need to remember, doctors are people too!
Going to the doctor can often times be daunting. Not only are you nervous about finding out whether or not you are healthy, but you also can be afraid that the doctor will judge you on your health, or more likely unhealthy, habits. However, you need to remember, doctors are people too! Hemorrhoids are a very common health problem, in which a lump or mass of tissue in the anus contains enlarged blood vessels. They are caused by an increase in abdominal pressure.
Hemorrhoids are a very common health problem, in which a lump or mass of tissue in the anus contains enlarged blood vessels. They are caused by an increase in abdominal pressure. Having a good understanding of your family’s health history is essential in disease prevention. Many of the most common and fatal disease can be hereditary, including heart disease, cancer and diabetes.
Having a good understanding of your family’s health history is essential in disease prevention. Many of the most common and fatal disease can be hereditary, including heart disease, cancer and diabetes.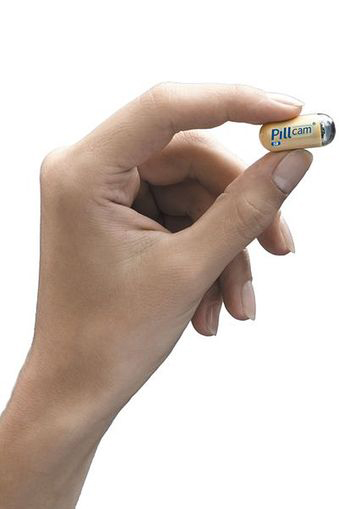 Endoscopy is a procedure that allows medical professionals to look inside your body. Instruments called endoscopes have cameras attached to long, thin tubes – which are inserted into various orifices of the body to examine nearby organs.
Endoscopy is a procedure that allows medical professionals to look inside your body. Instruments called endoscopes have cameras attached to long, thin tubes – which are inserted into various orifices of the body to examine nearby organs.
 As society becomes increasingly appearance-conscience, people are paying attention to parts of their bodies they had previously overlooked. While cosmetic surgery was most commonly used to improve and enhance the appearance of the face, the popularity of having elective cosmetic procedures has now spread throughout the body – most recently to the feet. A recent survey conducted by the American Orthopedic Foot & Ankle Society (AOFAS) among its
As society becomes increasingly appearance-conscience, people are paying attention to parts of their bodies they had previously overlooked. While cosmetic surgery was most commonly used to improve and enhance the appearance of the face, the popularity of having elective cosmetic procedures has now spread throughout the body – most recently to the feet. A recent survey conducted by the American Orthopedic Foot & Ankle Society (AOFAS) among its 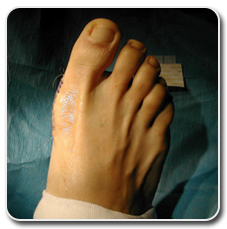 A bunion is the term given to a knot that appears on the side of the foot, just to the side of the lowest joint of the largest toe. The knot is made up of bone and soft tissue and appears when the largest toe has been pushed inward toward the other toes for an extended period of time. Heredity plays a role in bunion formation, as do illnesses such as arthritis and polio. However, the leading cause of bunions is wearing ill-fitting shoes where the toes are cramped together. Since women are more likely to wear poorly fitting shoes because of heels and such, bunions are more prominent in women. In fact, the American Orthopedic Foot and Ankle Society found that over 85 percent of women in the U.S. wear shoes that are too small and over 50 percent have bunions.
A bunion is the term given to a knot that appears on the side of the foot, just to the side of the lowest joint of the largest toe. The knot is made up of bone and soft tissue and appears when the largest toe has been pushed inward toward the other toes for an extended period of time. Heredity plays a role in bunion formation, as do illnesses such as arthritis and polio. However, the leading cause of bunions is wearing ill-fitting shoes where the toes are cramped together. Since women are more likely to wear poorly fitting shoes because of heels and such, bunions are more prominent in women. In fact, the American Orthopedic Foot and Ankle Society found that over 85 percent of women in the U.S. wear shoes that are too small and over 50 percent have bunions.
 A pterygium is a wing-shaped growth that can occur on the eye and eventually cover and alter the shape of the cornea. Pterygia consist of abnormal conjunctival tissue (the membrane that covers the eye) . Pterygia can be small or grow large enough to affect a person’s vision. It is not clear why pterygia form, but they are twice as likely to occur in males than in females and are most often found in people who live in eye-irritating environments, such as windy climates, smoky places or sandy tropical locations.
A pterygium is a wing-shaped growth that can occur on the eye and eventually cover and alter the shape of the cornea. Pterygia consist of abnormal conjunctival tissue (the membrane that covers the eye) . Pterygia can be small or grow large enough to affect a person’s vision. It is not clear why pterygia form, but they are twice as likely to occur in males than in females and are most often found in people who live in eye-irritating environments, such as windy climates, smoky places or sandy tropical locations.